A real-time EMS routing and decision support system for optimizing stroke patient transport and outcomes
This technology is a GPS-based device for ambulances that uses real-time patient data and hospital capabilities to guide EMS to the best stroke treatment center, improving outcomes by considering both travel time and the patient’s evolving condition.
Background
Stroke is a leading cause of death and long-term disability worldwide, necessitating rapid and precise medical intervention to minimize brain damage and improve patient outcomes. Emergency Medical Services (EMS) play a critical role in the early management of acute stroke by transporting patients to appropriate medical facilities. However, the landscape of stroke care is complex, with different hospitals offering varying levels of specialized treatment—Primary Stroke Centers (PSCs) provide initial assessment and thrombolytic therapy, while Comprehensive Stroke Centers (CSCs) are equipped for advanced procedures like Endovascular Thrombectomy (EVT) for large vessel occlusions (LVOs). The urgency of stroke treatment, encapsulated by the phrase "time is brain," underscores the need for EMS to make swift, informed decisions about hospital destinations to ensure patients receive the most effective care as quickly as possible. Current EMS routing protocols often default to transporting stroke patients to the nearest hospital, regardless of the facility’s capability to deliver the specific interventions required for different stroke subtypes. This approach can lead to suboptimal outcomes, particularly for patients with LVOs who may require immediate EVT—a treatment not available at all centers. Two main strategies exist: the "Drip and Ship" method, where patients are first taken to the closest PSC for assessment and initial treatment before being transferred to a CSC if necessary, and the "Mothership" approach, which involves direct transport to a CSC. Both strategies have limitations; the former can introduce critical delays due to inter-hospital transfers, while the latter may unnecessarily bypass closer facilities, potentially delaying treatment for non-LVO strokes. Additionally, current decision-making tools do not adequately account for the dynamic progression of stroke severity during transport or the real-time capabilities of nearby hospitals, leading to inefficiencies and variability in patient outcomes.
Technology Description
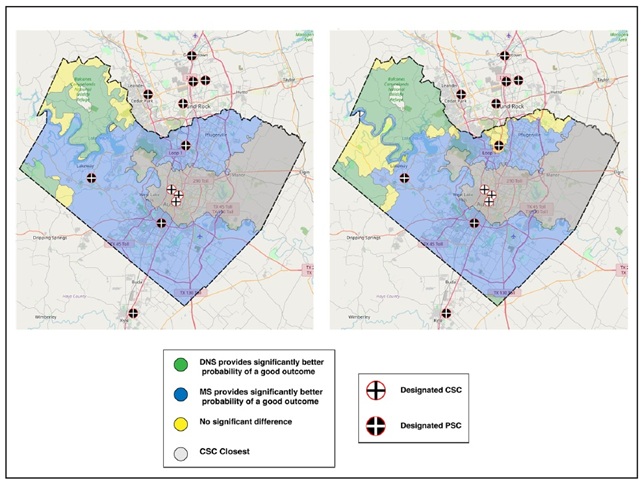
This technology is a GPS-based decision support device designed for Emergency Medical Services (EMS) to optimize the transport of acute stroke patients. By integrating GPS hardware with advanced arc-GIS mapping and a proprietary algorithm, the device continuously evaluates both transport times and predicted stroke outcomes to determine the most appropriate hospital destination—either a primary or comprehensive stroke center. The system dynamically assesses the evolving condition of the patient during transit, factoring in stroke severity and type to provide real-time routing recommendations. By leveraging a network of hospitals categorized by their stroke care capabilities, the device ensures that patients are directed to facilities equipped to deliver the necessary interventions, thereby reducing time-to-treatment and improving the likelihood of favorable outcomes. What differentiates this technology is its use of a physiological model to predict stroke progression, moving beyond traditional data-driven or epidemiological approaches. The device employs a mathematical framework that models infarct core growth as an exponential function influenced by collateral blood flow, allowing it to account for the unique evolution of each patient’s stroke. This is particularly critical for large vessel occlusions (LVOs), which require specialized treatment only available at comprehensive stroke centers. Through extensive simulations, the system evaluates various transport strategies, such as Drip and Ship versus Mothership, to determine the optimal approach based on real-time patient data and hospital capabilities. This integration of physiological modeling with real-time geographic and clinical data provides EMS personnel with a tailored, evidence-based tool that can significantly improve stroke care outcomes and streamline emergency response protocols.
Benefits
- Optimizes ambulance routing by integrating real-time GPS data with stroke severity and type to select the most appropriate hospital.
- Improves patient outcomes by reducing time-to-treatment and ensuring transport to facilities equipped for specific stroke care needs.
- Incorporates advanced physiological models predicting stroke progression, enabling tailored transport decisions beyond traditional methods.
- Utilizes arc-GIS mapping to continuously monitor stroke evolution during transport for dynamic route adjustments.
- Supports EMS personnel with a versatile tool that categorizes hospitals by stroke care capability, enhancing decision-making.
- Reduces unnecessary hospital transfers by directing patients to the optimal stroke center initially.
- Demonstrates effectiveness through extensive simulations, validating improved outcomes in various geographic regions.
- Represents a significant advancement in emergency medical services technology with potential to revolutionize stroke treatment protocols.
Commercial Applications
- EMS ambulance stroke routing optimization
- Hospital network stroke triage integration
- Real-time stroke outcome prediction
- Regional stroke care coordination
Opportunity
Available for co-development or exclusive license
Patent PCT/US2022/027010
US National patent filed

